In this week’s Sundays with Seegers, County Commissioner candidate Jake Seegers questions why county leaders appear poised to expand public messaging around harm reduction instead of reexamining outcomes. With talk of a Public Information Officer and efforts to counter “misinformation,” he asks whether taxpayer dollars are going toward optics rather than reform. Seegers highlights disputed syringe data and the contrast between supply distribution and treatment-focused efforts like Operation Shielding Hope — arguing residents want measurable results, not better messaging.
Clallam County citizens are aware, engaged, and activated like never before. They are demanding accountability, transparency, and measurable results from local leadership. The status quo is being challenged.
For more than a decade, harm reduction and Housing First initiatives have defined county policy. At the same time, leadership has been unwilling to directly address the social and ecological catastrophe of long-term outdoor living in public spaces. The result is a growing perception that Clallam County has become a place of least resistance for substance abuse and homelessness.
Rather than acknowledge failure and pivot toward common-sense course correction, entrenched officials appear to be defending the same policies that produced the current conditions.
Recently, that defense has crystallized around a simple strategy: discredit dissent by labeling it “misinformation.”
Commissioners, departments, committees, and county-funded NGOs increasingly frame public criticism as confusion from concerned but misinformed constituents.
At the February 3rd, 2026 Homelessness Task Force meeting, members proposed forming a subcommittee to craft a “State of Homelessness” presentation for both commissioners and the public. The stated purpose was to address “significant misconceptions” about homelessness funding and to develop a “unified, accurate, and compelling message” aligned with the county’s five-year plan.
At the February 17th Board of Health meeting (timestamps are included in the article), Commissioner Ozias sought advice from Health Officer Allison Berry and Health and Human Services (HHS) leadership about hiring a Public Information Officer to better communicate county initiatives (1:26:30).
In other words, even while forecasting multi-million-dollar financial deficits, commissioners are exploring spending taxpayer money to fund a position whose primary function would be to explain to taxpayers why current county policies are working.
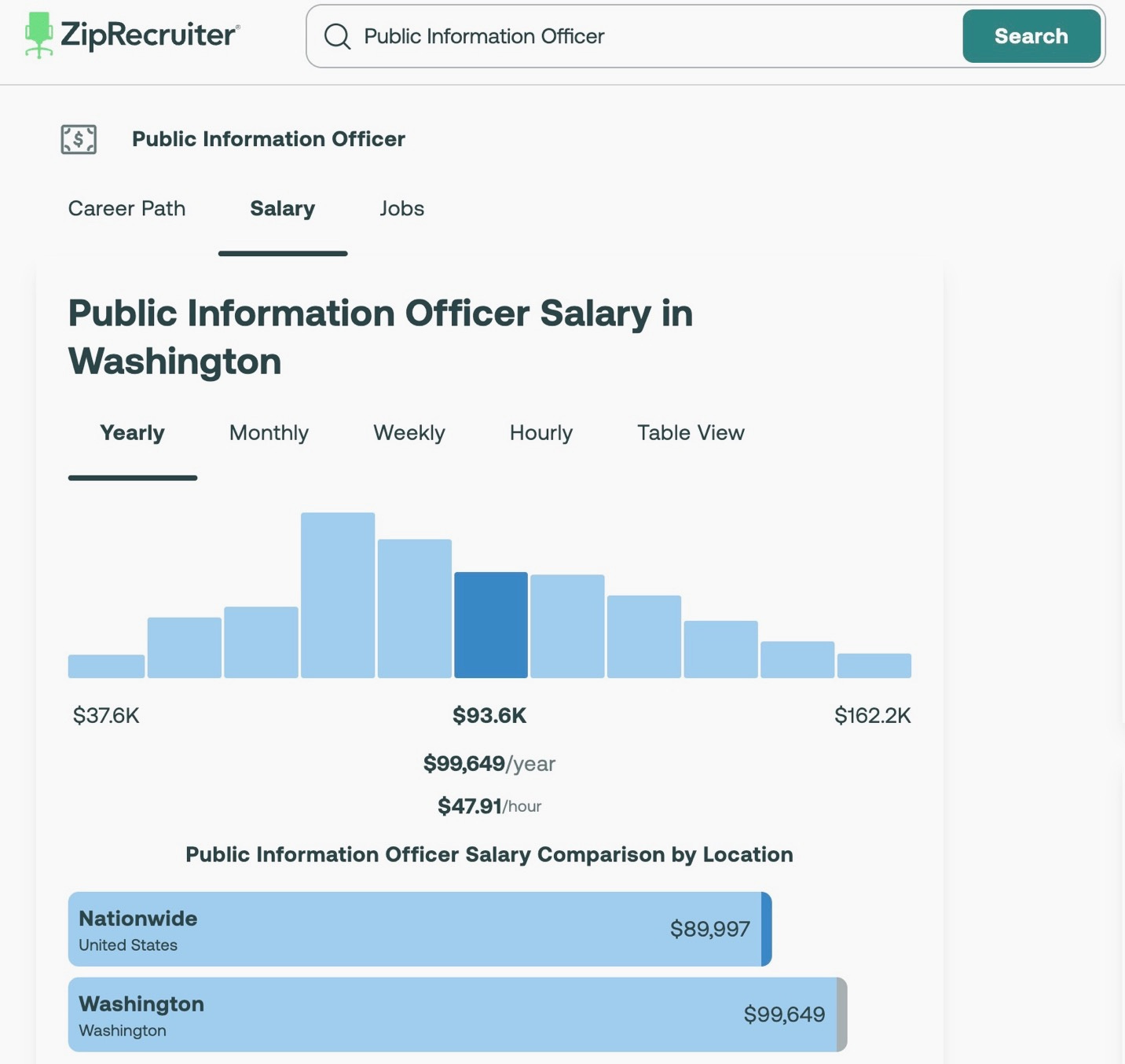
ZipRecruiter estimates the average Public Information Officer salary in Washington at roughly $100,000 annually. With benefits and overhead, that position could easily approach $150,000 per year.
That is a significant price tag for a role tasked with managing perception rather than correcting outcomes.
Commissioner Ozias’ request for advice on improving the county’s public messaging came on the heels of an extensive pro-harm-reduction presentation by Health Officer Allison Berry.
Throughout her remarks, Dr. Berry repeatedly invoked phrases such as “gaps in information,” “fundamental misunderstanding,” “conflation,” and “misinformed” to characterize community concerns. The cumulative effect was not simply to clarify policy, but to frame opposition as rooted in confusion rather than in legitimate disagreement over outcomes.
Syringe Summation
Just minutes before suggesting that private citizens removing syringes from the banks of Tumwater Creek is an act of theft, Health Officer Berry presented what she described as “data” on syringe distribution and return counts (58:50):
“Syringe service programs are known to reduce needle litter… We take in more syringes than we put out into the community.”
She reported that in 2024:
90,948 syringes were distributed
122,407 syringes were taken in
Net decrease: 31,459 syringes
The commissioners seemed impressed.
Commissioner Johnson responded, “I’ve been told exactly the opposite.”
Berry replied emphatically: “I know, but look at those numbers. They’re right there!”
However, one critical question went unasked by the commissioners: How are returned syringes counted?
Distribution is straightforward. Syringes are handed out in pre-packaged bundles that are easy to tally.
Returns are different. Syringes are not counted individually. Instead, they are estimated by container size.
If a container is logged as “full,” it is credited with a predetermined number of syringes.
That system may protect staff safety, but it also introduces upward bias. If containers are not filled to capacity, total return counts could be significantly inflated.
The stated container capacities also appear to be rough estimates rather than precise measurements. According to the chart, a 2-gallon sharps container holds 550 syringes — yet a 1-gallon container reportedly holds more than half that amount. A 1-liter bottle (nearly 34 ounces) is credited with 70 syringes, while a smaller 30-ounce detergent container is listed at 80.
In a simple spot test, it required the determination of force to compress 36 syringes into a 20-ounce Gatorade bottle labeled with a stated capacity of 40.
Even using a transparent container, it would be difficult to distinguish between 25 and 35 syringes by visual inspection alone — both could reasonably be deemed “full” and credited with the chart’s 40 syringe capacity.
These discrepancies invite a straightforward question: Are more syringes actually being removed than distributed?
The visible increase in needle litter across public spaces has led some residents to question that claim.
When return totals are calculated using estimated container capacity rather than individual counts, even small assumptions about how full a container is can compound — potentially adding up to tens of thousands of syringes over the course of a year.
Numbers built on estimates rather than direct verification deserve careful review, especially when they’re used to dismiss public concern.
At the same time, local cleanup nonprofit 4PA reports collecting and returning more than 12,000 discarded syringes across 2024 and 2025 from public lands. According to the organization, each syringe is counted individually.
Dueling Dashboards
This is not the first time Health Officer Berry has relied on debatable data to support the efficacy of her harm reduction policies. In a January 2019 article in the Peninsula Daily News, Berry stated that 2018 overdose deaths had declined due to expanded naloxone access.
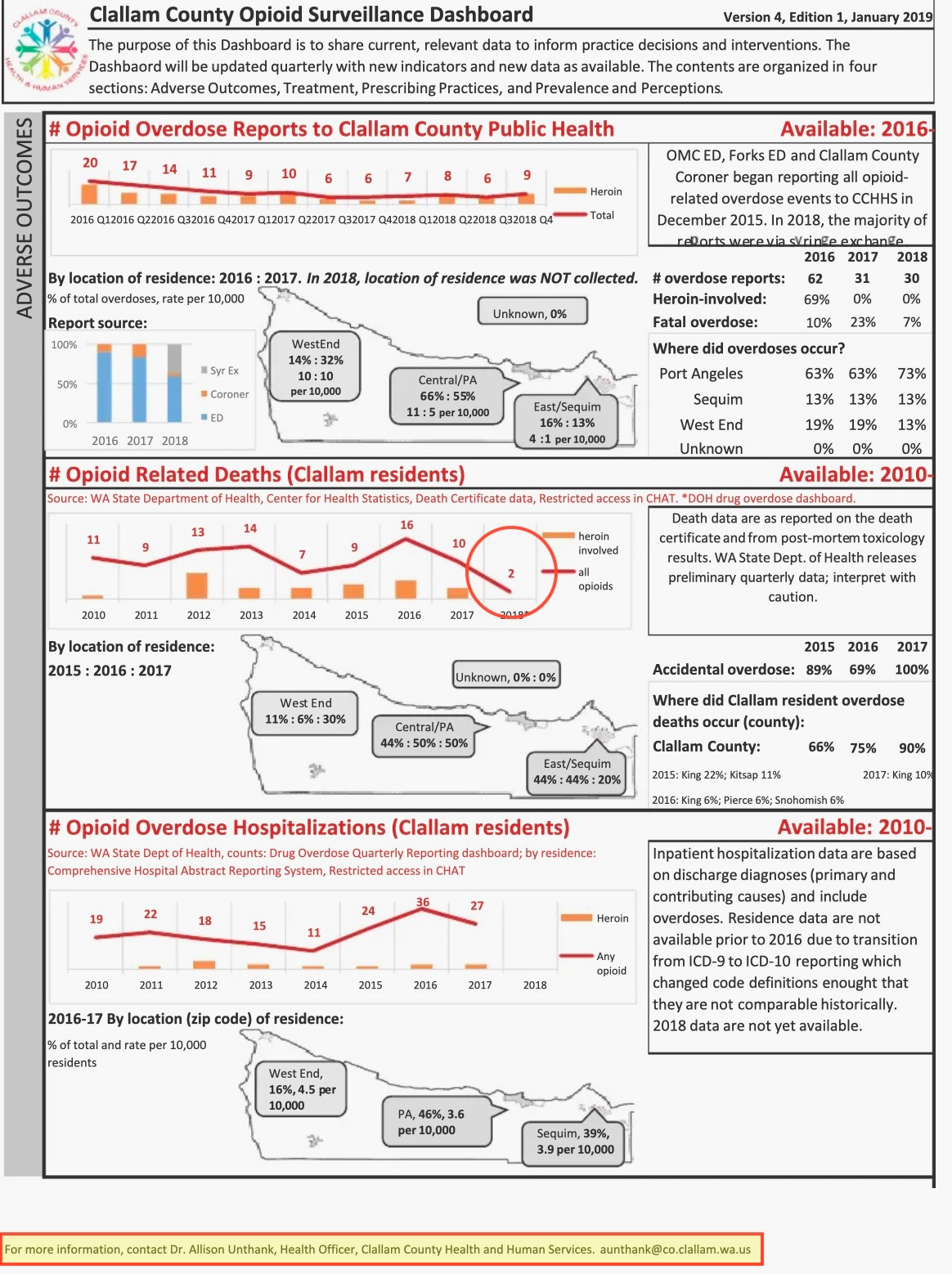
The article reported a drop from 10 overdose deaths in 2017 to just 2 in 2018, citing an “Opioid Surveillance Dashboard” compiled by Dr. Berry and HHS.
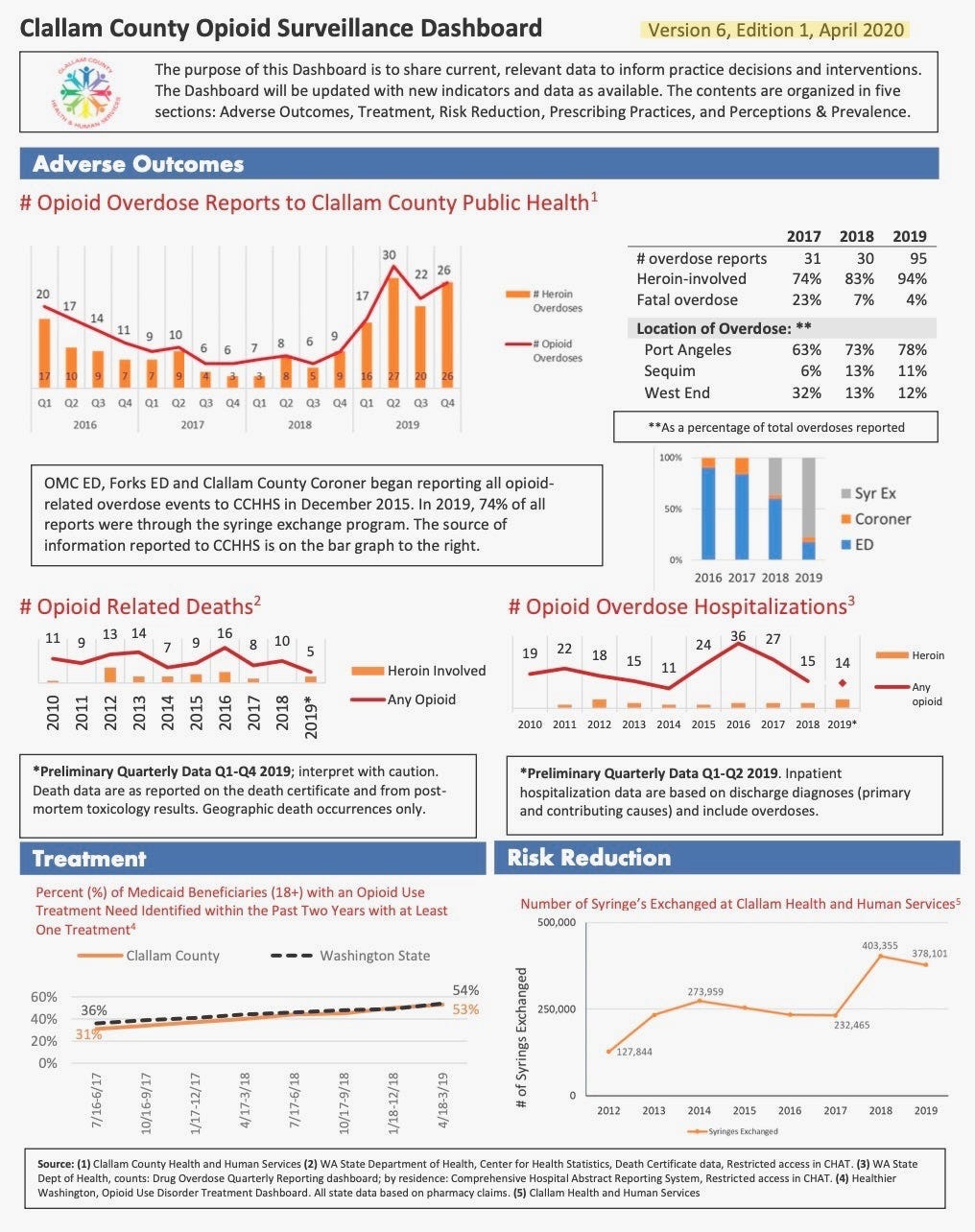
However, only three months later, the dashboard was updated to show 10 overdose deaths in 2018 — not 2 — indicating an increase rather than a decrease from the prior year.
More recently, Deputy Coroner Rebecca Shankles conducted a case-by-case review and revised the verified 2018 total to 8 overdose deaths.
When headline figures shift so dramatically over time, it raises legitimate questions about the reliability of the data used to declare policy success. Each revision chips away at public trust.
That erosion of public confidence makes the commissioners’ decision to allocate $25,000 for HHS to produce its own “Gaps Report” particularly concerning. When the same department that designed and implemented the policies is tasked with evaluating their effectiveness — and shaping recommendations for future funding — questions about independence and objectivity are inevitable. Even if the work is done in good faith, the structure itself invites skepticism.
The Harm Reduction Victory Lap
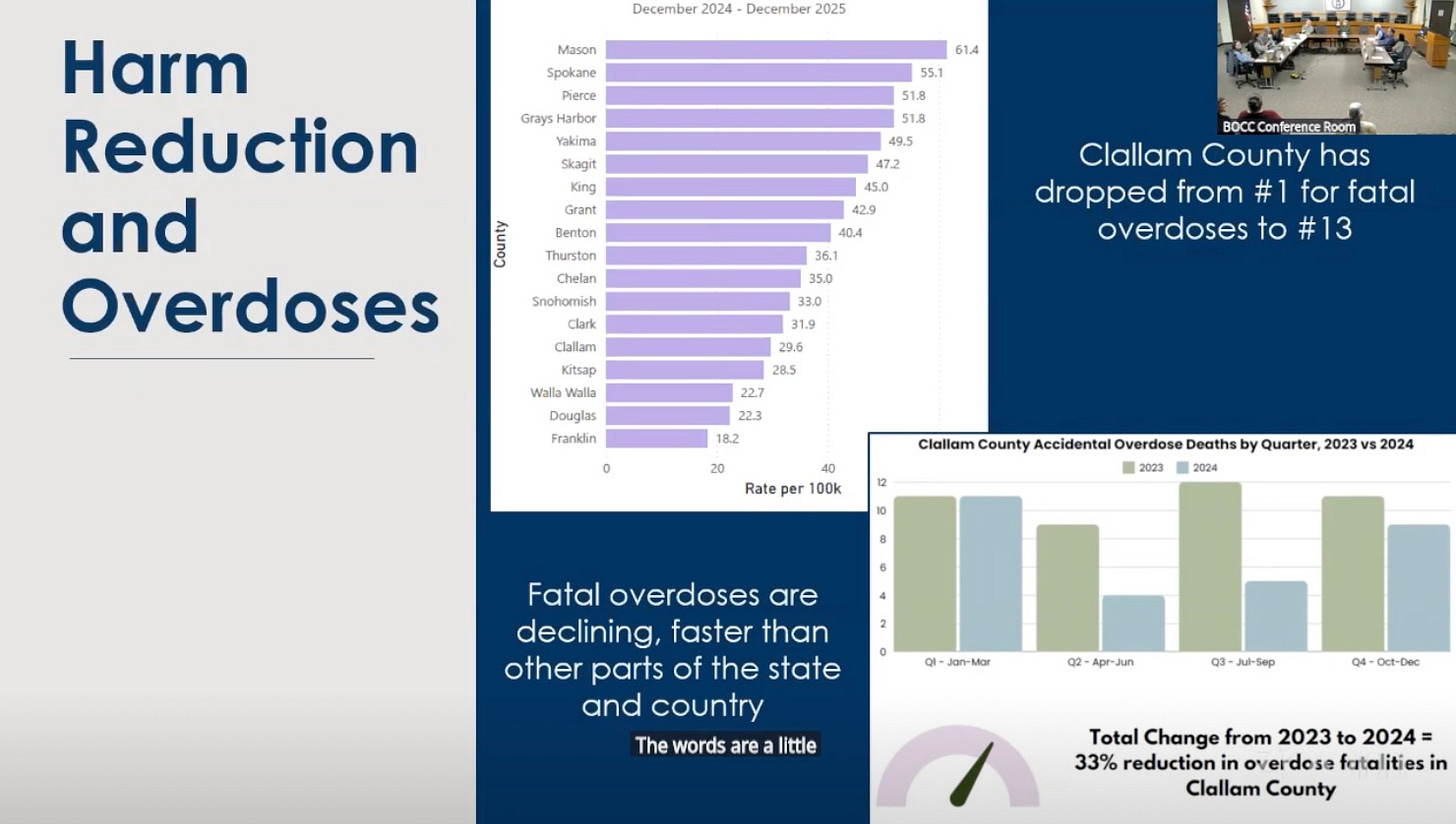
Dr. Berry claimed a win for harm reduction by citing a 33% reduction in overdose deaths in 2024. According to Clallam County’s Deputy Coroner, 2025 overdose fatalities dropped by another 19% to 25 total.
These reductions in overdose deaths are welcome.
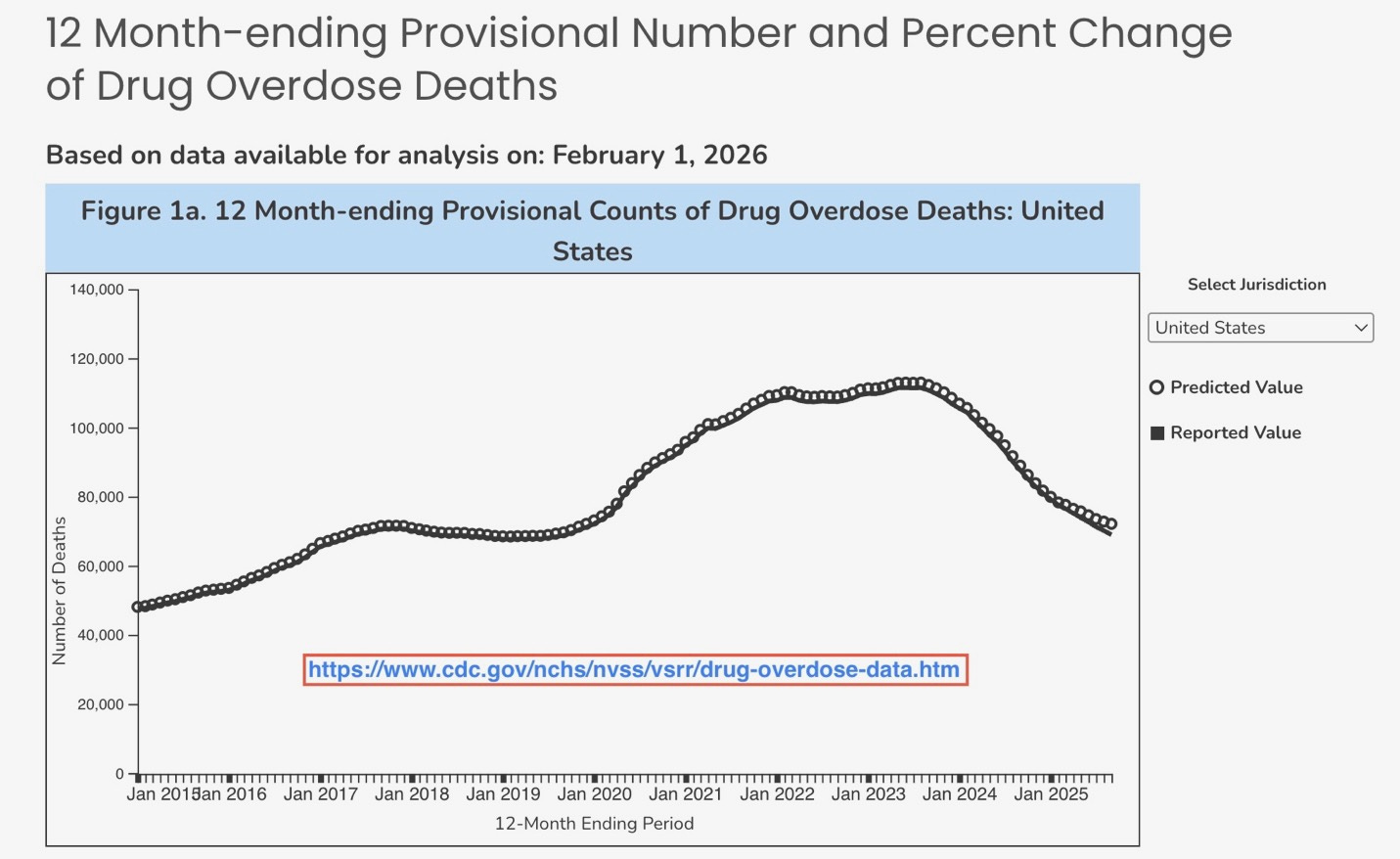
But the declines track national trends. The Centers for Disease Control and Prevention reported that U.S. overdose deaths fell approximately 27% in 2024, followed by another provisional decline of more than 23% in the 12-month period ending August 2025.
Clallam’s decline mirrors the broader pattern.
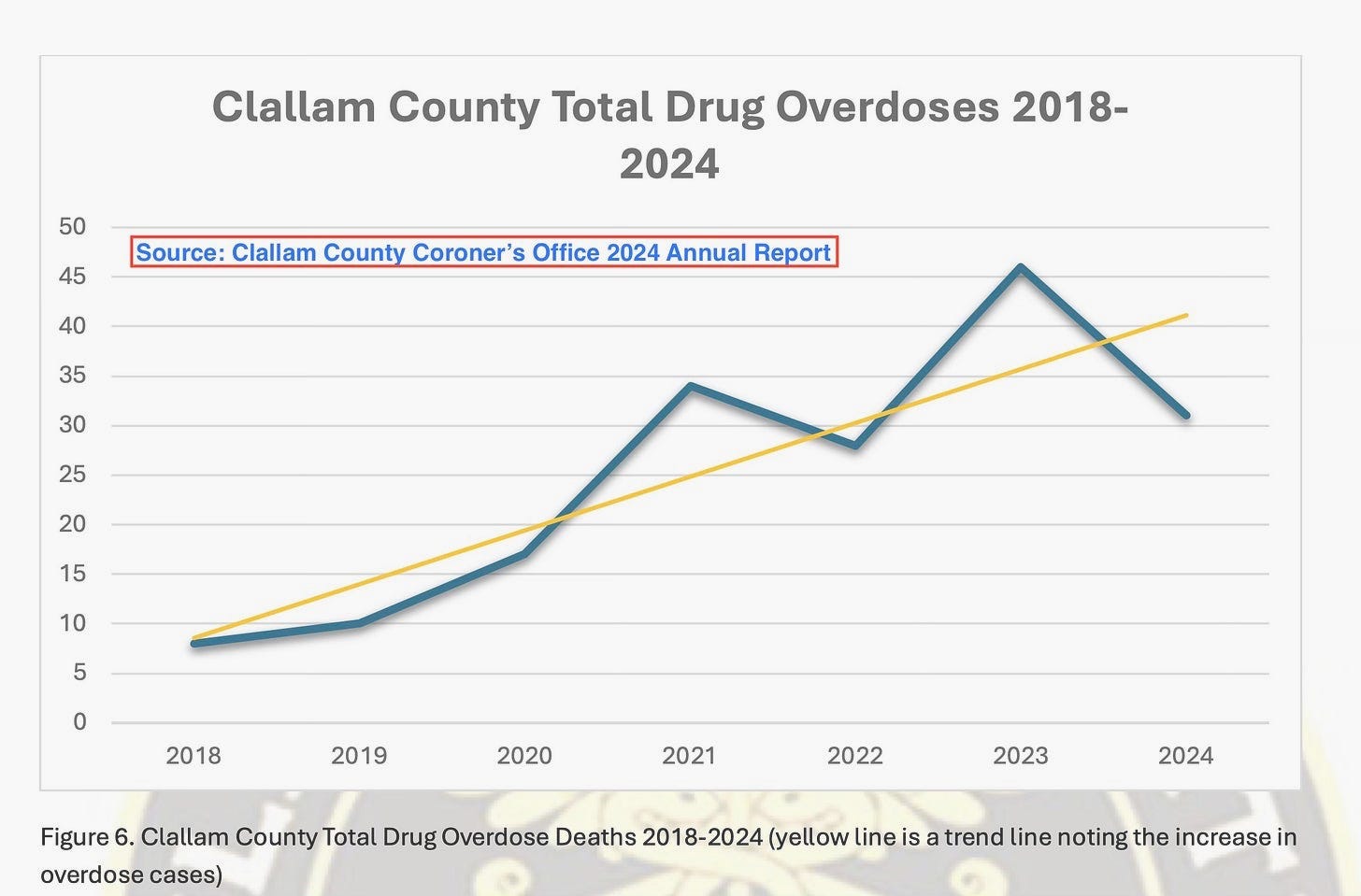
What Dr. Berry refuses to take credit for is the surge in overdose deaths from 2018 to 2024, when fatalities in Clallam increased by more than 500% before reaching a 12-month peak in March of 2024 (according to the Coroner’s Office).
Even after two consecutive years of decline, overdose deaths in Clallam County remain roughly triple the 2018 levels.
That is not a victory-lap statistic. It is evidence of a local epidemic that unfolded under the tenure of the Health Officer and the commissioners who have fueled Clallam’s harm reduction expansion.
The Harm Reduction Lifeline
Yet, despite harm reduction’s abysmal record in Clallam County, Dr. Berry continues to label dissenters as “misinformed,” and she clings to its effectiveness (57:20):
“It’s working. It’s keeping people alive, and to stop will very likely lead to an increase in overdoses in our community rather than a reduction.”
Dr. Berry cited reported reductions to harm reduction programs in Spokane, Mason, and Grays Harbor counties — followed by increases in overdose deaths — as evidence that scaling back those services can lead to worse outcomes.
That conclusion, however, overlooks the broader context in which those policy changes occurred. Counties that expanded harm reduction efforts over many years may already have been facing widespread fentanyl availability and deeply entrenched addiction. In that kind of environment, any shift in policy — whether expanding or scaling back services — happens against a backdrop of already heightened risk, making simple cause-and-effect conclusions harder to draw.
A more appropriate comparison would examine jurisdictions that significantly restricted the distribution of drug-use supplies from the outset. In states such as Alabama, Kansas, Missouri, Mississippi, Nebraska, South Dakota, and Wyoming, syringe services programs (SSPs) have historically been illegal or effectively prohibited. While SSPs are technically legal in Idaho and Texas, they operate under tighter constraints, and the distribution of other drug-use supplies is restricted.
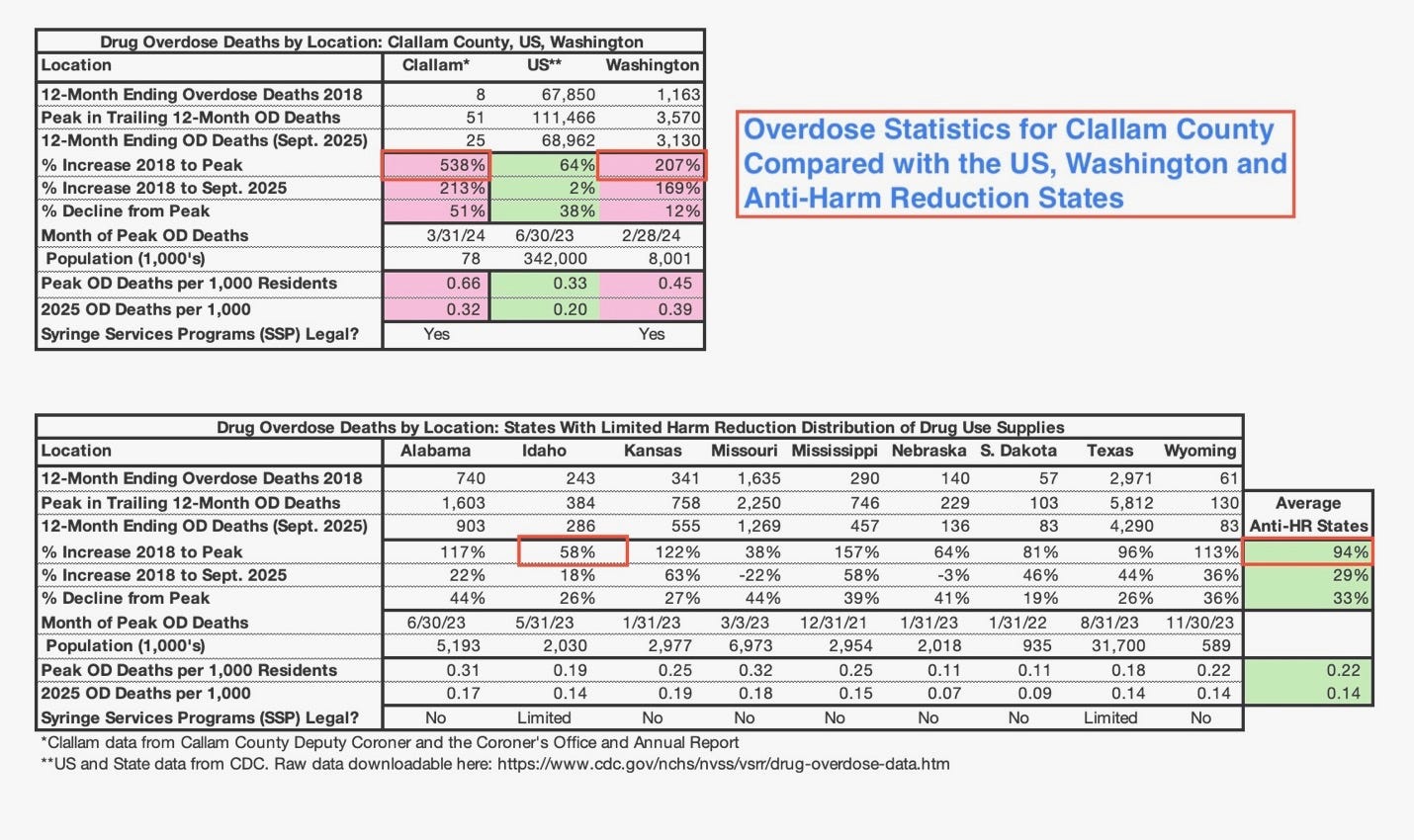
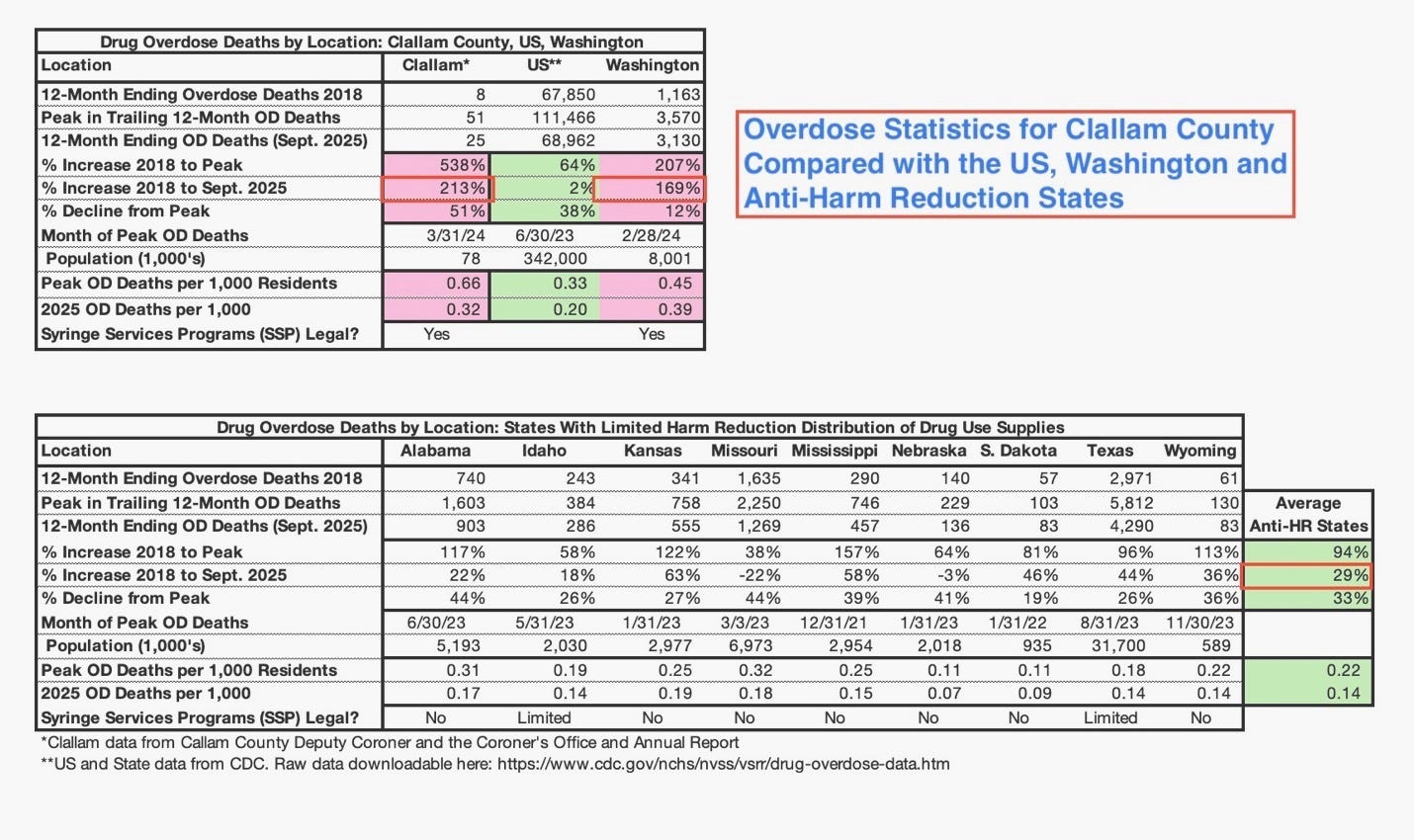
The table below was compiled using data from the Clallam County Coroner’s Office and the CDC. It compares Clallam County with the United States overall, Washington State, and states that have resisted or significantly limited the distribution of drug-use supplies under harm reduction policies.
Specifically, the table examines:
The percentage increase in annual overdose deaths from 2018 to each location’s 12-month peak.
The percentage decline from each location’s peak to current levels.
The net percentage increase in annual overdose deaths from 2018 to the present, even after the recent nationwide decline.
Overdose deaths per 1,000 residents for each location.
Together, these metrics provide a clearer picture of both the surge phase and the post-peak correction — as well as the overdose death frequency relative to population size.
From 2018 to peak levels:
Washington State overdose deaths increased by 207%.
Clallam County increased by 538%.
States with strict or prohibited syringe programs saw smaller percentage increases, averaging increases of 94% - less than half of WA state’s trajectory and less than 1/5 of Clallam’s.
Idaho, Washington’s eastern neighbor with significantly more restricted harm-reduction infrastructure, experienced a comparatively smaller 58% increase in overdose deaths, reaching its annualized peak roughly ten months before Clallam County.
As of late 2025, overdose deaths in those stricter states are still higher than they were in 2018. However, their increases have been significantly smaller than the proportional rises seen in Washington overall — and in Clallam County specifically.
Clallam County’s 25 overdose deaths in 2025 are still more than triple the 8 overdose deaths reported by the Coroner’s Office in 2018.
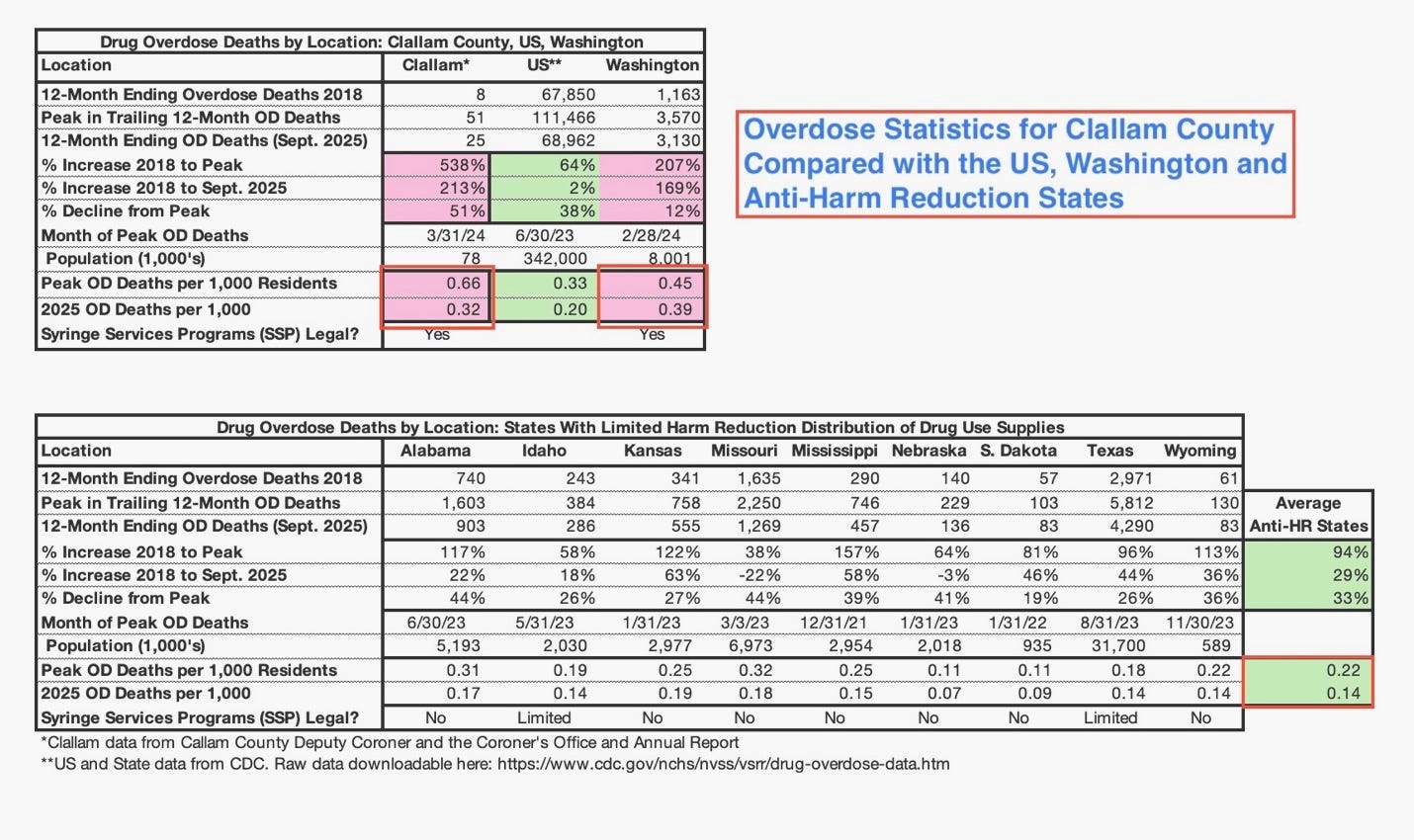
Also of note, Clallam’s overdose deaths per 1,000 residents remain more than double those of Idaho and higher than the average among states that strictly limit syringe distribution.
In other words, although Clallam’s annual overdose deaths have declined over the past two years, they remain roughly three times higher than in 2018. That proportional increase exceeds Washington’s overall trajectory and is significantly higher than states that prohibit or tightly restrict the distribution of syringes and other drug-use supplies. Both Washington and Clallam continue to exhibit notably higher overdose fatality rates per 1,000 residents compared with jurisdictions that maintain stricter limits on harm-reduction infrastructure.
While Health Director Berry and the commissioners highlight Clallam’s recent reduction in overdose deaths, they rarely acknowledge that the years during which syringe service programs and “safe-use supplies” were aggressively expanded also coincided with an eight-year surge in fatalities — a trajectory steeper than that experienced in several states that maintained stricter limits on such programs.
What has worked?
It strains credibility to argue that harm reduction suddenly became effective after a decade of worsening outcomes. A more plausible explanation for the recent decline in overdose deaths may lie in targeted treatment engagement efforts rather than continued supply distribution.
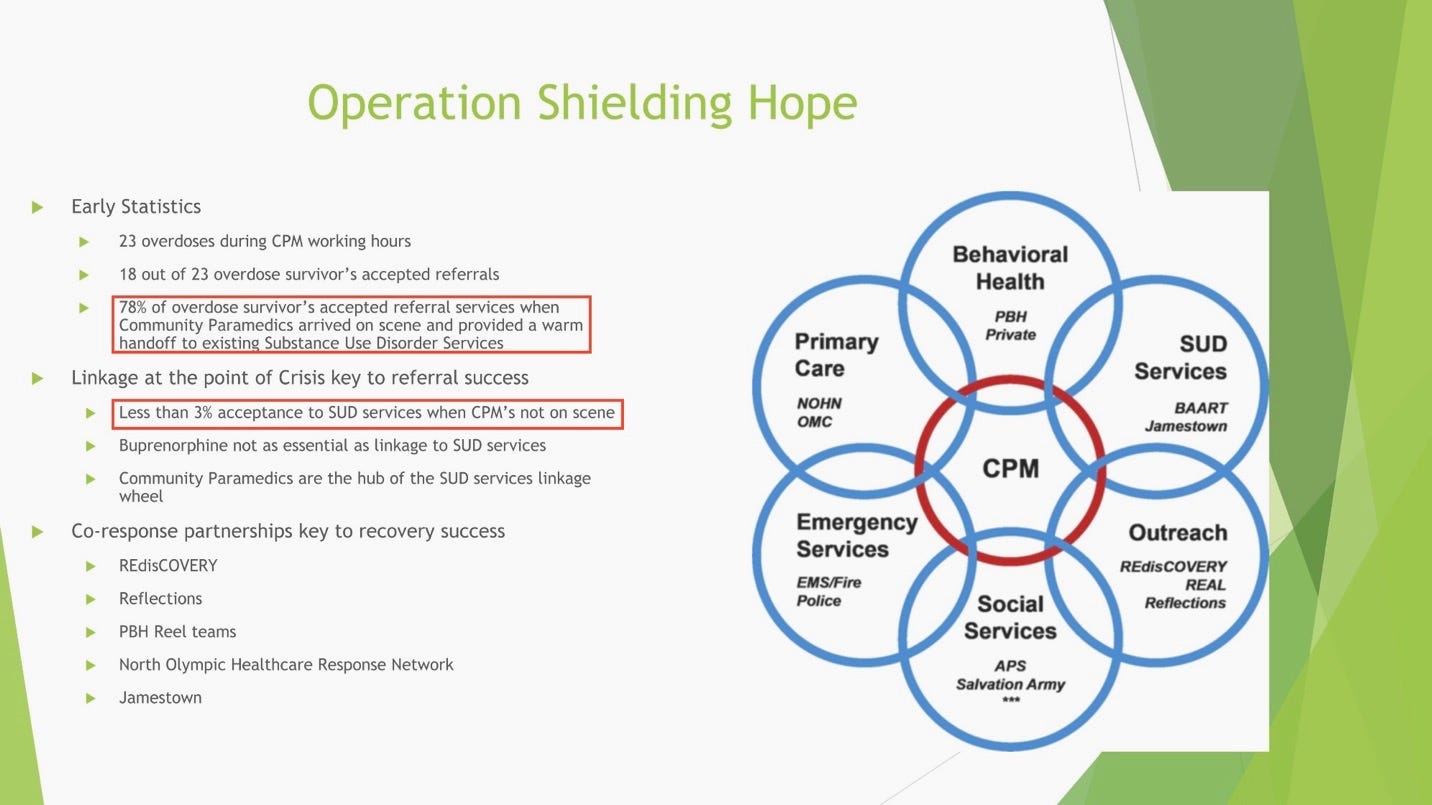
In March 2024 — at the height of Clallam’s overdose death rate — the Port Angeles Fire Department launched Operation Shielding Hope. The program differs fundamentally from traditional harm-reduction strategies. Instead of focusing on distributing supplies or facilitating “safer” drug use, it intervenes at the critical moment immediately following an overdose to connect individuals directly to treatment and recovery pathways.
Community paramedics respond after overdoses, stabilize patients, and build rapport in real time.
According to PAFD Chief Sharp, 78% of overdose survivors accepted referral services when community paramedics were involved, compared with fewer than 3% when that follow-up engagement did not occur.
If overdose deaths are declining, it’s fair to ask whether programs that move people into treatment — rather than simply maintaining them in active use — are contributing in a meaningful way.
Treat with Drugs Instead of Detox
Countless recovery testimonials from individuals such as Chelsea Jones, Ron Davis, Ginny Burton, and Jenni Tiderman-Rogers emphasize the pivotal role that jail or structured inpatient treatment played in their sobriety. For many, separation from environment — not medication — was the turning point.
During her presentation, Dr. Berry acknowledged that inpatient treatment capacity statewide is limited, describing waiting lists as “massive.” She added (30:30):
“Inpatient is not necessary for everybody. A lot of people can do well outpatient.”
Accordingly, she has prioritized rapid outpatient access — often within 24 hours. The outpatient model she highlighted centers on medication-assisted treatment using buprenorphine (Suboxone) and methadone (28:40):
“We’ve done a lot of work to increase outpatient treatment. So, it’s a lot easier to get buprenorphine than it used to be. Most of our primary care clinics offer buprenorphine, also known as Suboxone… We have two sites in the county that currently offer methadone maintenance — Jamestown and BART — and they are much easier to get into. They generally will do same-day evaluations for folks and that can be really critical.”
The policy choice is clear: expand access to outpatient medications rather than invest heavily in structured inpatient capacity.
Critics argue that this approach effectively substitutes one opioid for another while leaving individuals in the same destabilizing environments. The irony is difficult to ignore: several pharmaceutical manufacturers that now produce buprenorphine and methadone products were defendants in nationwide opioid litigation and agreed to substantial settlement payments for their role in the opioid crisis (e.g., Teva and Hikma). Today, Clallam County purchases those same medications and classifies their ongoing use as treatment.
Expansion of Drug Use
Health Officer Berry is adamant that distributing safe-use supplies does not increase drug use (39:20).
“This idea that giving people safe-use supplies somehow makes them use more is a fundamental misunderstanding of how drugs work. People don’t use drugs because of the pointy end… they use drugs because of the drugs.”
Yet some individuals in recovery dispute that claim. Chelsea Jones, for example explained that access to clean needles and pipes encouraged drug use:
“In the moment, it was probably — I thought it was helpful — because now I had a roof over my head and they delivered all my drug-using supplies right to my door — I didn’t even have to go anywhere… it didn’t help my substance use, it just enabled that. It made that super easy.”
In December, the Peninsula Daily News quoted Dr. Berry as saying, “Statistically, only one in five [homeless] have substance use disorders.” Then, during the February 17 Board of Health presentation, she stated that only about one-third of people living outside are using drugs.
Those assertions contrast starkly with what many residents observe firsthand. In interviews conducted along Tumwater Creek, nearly every one of the 15 individuals spoken with acknowledged current drug use while living outdoors. One young man put it bluntly: “Everybody has to use out here. If you’re homeless, you have to use to survive.”
More broadly, many Clallam residents report a visible expansion of the open-air drug economy and public drug use. Transactions in downtown Port Angeles, including near the fountain, have been documented by concerned citizens, followed by open consumption.
A transaction near the Port Angeles downtown fountain was captured by a concerned citizen, followed by open drug use (pictured below).
Residents also regularly report erratic and dangerous behavior consistent with heavy methamphetamine use.
Dr. Berry describes much of this as meth-induced psychosis and offered this perspective (33:40):
“When you see someone on the street who’s shouting at somebody who doesn’t appear to be there, often the solution to that is not jail. It’s a sandwich and a water and a quiet place to be.”
Will current leaders turn Clallam into the next Seattle?
Demanding Change
Clallam County’s citizens are not confused. They are not suffering from a “fundamental misunderstanding.” They are responding to what they can see with their own eyes — eight years of escalating overdose deaths, expanding public drug use, mounting needle litter, and a growing sense that policy has drifted far from accountability.
Yes, overdose deaths have declined over the past two years. That is good news. But declines that mirror national trends do not automatically validate a decade of local strategy — especially when that same strategy coincided with a more than 500% increase in fatalities before the peak.
If harm reduction were the decisive solution, the surge should never have reached those levels.
At the same time, programs like Operation Shielding Hope demonstrate that immediate engagement and treatment referrals can lead to measurable participation in recovery pathways. That model emphasizes transition out of addiction — not long-term maintenance within it.
The debate in Clallam County is not about compassion. It is about outcomes.
It is not about whether people struggling with addiction deserve help. They do.
It is about whether the policies chosen by local leadership have reduced addiction, reduced disorder, and reduced death — or simply managed and normalized them.
When commissioners consider hiring a Public Information Officer to shape the narrative, and when departments commission internal “Gaps Reports” to evaluate their own policies, citizens reasonably question whether the priority is reform — or reputation management.
Public trust cannot be rebuilt with better messaging.
It will be rebuilt when:
Data is transparent and methodologically sound.
Success is measured by outcomes, not inputs — tracking how many individuals transition from addiction to sobriety.
Failures are acknowledged without defensiveness.
Policy shifts follow evidence rather than ideology.
Clallam County stands at a crossroads.
It can continue defending the framework that produced years of escalating fatalities and visible disorder, or it can recalibrate toward policies that prioritize recovery, accountability, and measurable improvement in public safety and public health.
The public is no longer passive.
They are watching the numbers.
They are watching the streets.
And they are demanding results.
What Can You Do?
If you were in charge, would you invest in better messaging — or demand better results?
Clallam County residents deserve clear answers, independently verified data, and measurable proof that current policies are reducing addiction, disorder, and death.
Now is the time to speak up.
Contact the Board of County Commissioners through the Clerk of the Board at loni.gores@clallamcountywa.gov and ask that your message be shared with all three commissioners. Email Dr. Allison Berry directly at allison.berry@clallamcountywa.gov.
Ask them:
Are syringe returns individually counted or estimated?
How many people have moved from addiction into sustained recovery?
Why consider a Public Information Officer during a budget deficit?
What benchmarks would trigger a change in policy?
Public trust depends on transparency and accountability.
Make the call. Send the email. Ask the questions.
Last week, Jake Seegers asked readers what local government should do first after seeing the conditions along Tumwater Creek. Of 176 votes:
72% said, “Eliminate outdoor living”
13% said, “Create an outdoor camping area”
10% said, “Expand shelter capacity”
5% said, “Place anti-panhandling signs”
No one thinks the current policies are working
Editor’s Note: CC Watchdog editor Jeff Tozzer also serves as campaign manager for Jake Seegers during his run for Clallam County Commissioner, District 3. Learn more at www.JakeSeegers.com.